Welcome Our Newest CSI Team Member

Joy Perrin, BSN, RN, CCRN, Clinical Simulation Educator
Joy earned a Bachelor of Science in Nursing from the Medical College of Georgia in 2005. She also holds an associate degree in business from Truett McConnell College and a Bachelor of Science in biology from Piedmont University.
With more than 20 years of experience as a registered nurse, Joy began her career at Northeast Georgia Health System (NGHS) in the cardiovascular intensive care unit as a nurse extern. She recently celebrated her 20-year anniversary as an RN.
Throughout her career, Joy has developed extensive expertise in critical care nursing, serving in roles including CVICU/CCU charge nurse, critical care flex pool nurse, nurse preceptor and assistant nurse manager. Her dedication to patient care has been recognized at the Regional STEMI Summit for her compassion, empathy and clinical excellence. During the COVID-19 pandemic, she played a key role in opening and staffing the COVID ICU and has been an active member of the Rapid Response Team since its inception at NGHS.
Most recently, Joy served as assistant nurse manager of NGHS’s Central Monitoring Unit, a pioneering program in Georgia that monitors more than 500 patients across five campuses from one centralized location. She is certified by the American Association of Critical-Care Nurses as a Critical Care Registered Nurse (CCRN).
In her current role as a clinical education simulator, Joy specializes in graduate medical education, developing simulation scenarios and procedures for internal medicine and critical care physician residents. She also provides simulation-based education and training for nurse residents and patient care technicians.
Advanced Critical Care Simulation Rotations Begin for 2025-2026 Academic Year
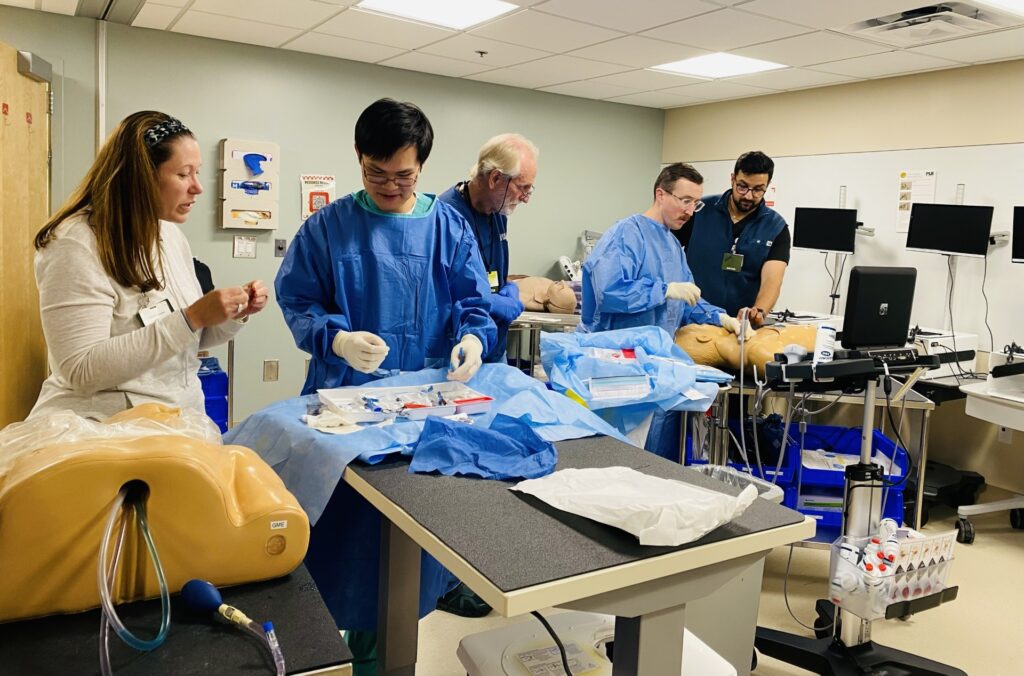
August marks the start of our Advanced Critical Care simulation rotations for the 2025–26 academic year, offering essential hands-on training for residents currently in critical care rotations. Held on the second and third Friday of each month, these intensive sessions present residents with complex scenarios they are likely to encounter in real clinical settings.
The program provides valuable opportunities for residents to practice a wide range of critical procedures in a safe, controlled environment before performing them in actual care units. Dr. Brandon Gordon, critical care chief, coordinates the scheduling to ensure optimal participation and learning outcomes. This structured approach to simulation-based education reinforces our commitment to preparing the next generation of critical care physicians with the skills and confidence needed to excel in high-stakes medical situations.
Step Inside the Future of Healthcare Training: New Video Tour Showcases Lanier Park Learning Lab
The Northeast Georgia Health System’s Center for Simulation and Innovation has released a new immersive video tour that guides new hires and learners through the Lanier Park Learning Lab in Gainesville, Georgia. This state-of-the-art facility includes 10 specialized patient simulation rooms—Medical, ICU, NICU, LDRP, PACU and OR—each equipped with high-fidelity simulation manikins operated from advanced control rooms.
The video showcases lifelike manikins with features such as dilating eyes, realistic breathing patterns and speaking capabilities, creating a highly realistic training environment. The Center promotes high-quality, safe patient care through excellence in multimodal simulation-based training and experiential learning. Its vision is to be a global leader in simulation education while enhancing team performance and communication.
Medical Education Innovates with Escape Box Learning for ABIM Board Preparation

The Center for Simulation and Innovation partnered with Meghan Bratkovich, Ph.D., M.Ed., M.A., medical education faculty development specialist, to deliver an innovative educational experience during the Internal Medicine PGY-3 and chief resident retreat. The collaboration introduced ABIM board prep escape boxes, transforming traditional board review into an engaging, team-based learning activity.
The escape boxes covered essential clinical scenarios—including acute limb ischemia, asthma exacerbations, diabetes management and gallstone pancreatitis—as well as professional development topics such as maintenance of certification and DEA training requirements. Teams of up to five participants worked together to solve puzzles and unlock sequential containers within a 30-minute time limit.
The winning team—Brady Chen, Cinsley Gentillon, Miriam Nji, Cindy Idowu, Femi Olukayode and Katherine Keck—demonstrated exceptional teamwork and clinical knowledge, completing the challenge in the fastest time. The activity exemplified how simulation-based learning can enhance board preparation while fostering collaborative problem-solving skills essential for clinical practice.
NGMC Cardiovascular Disease Fellows Excel in Comprehensive Simulation Training
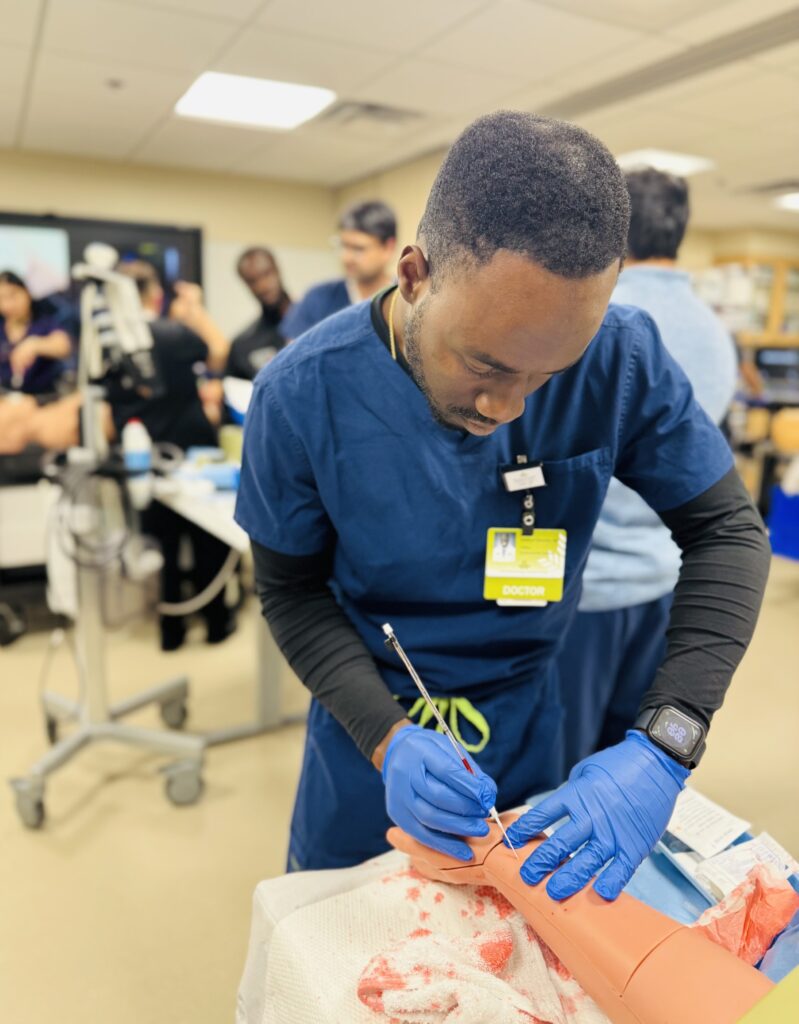
NGMC Cardiovascular Disease Fellows recently participated in an intensive simulation day at GME, with 14 fellows attending to enhance their procedural skills across multiple critical competencies. The comprehensive training session focused on essential cardiovascular procedures and diagnostic techniques, including Central Venous Catheter (CVC) placement, arterial line insertion, Vimedix ultrasound simulation, and Harvey cardiac examination training. This hands-on simulation experience provided our cardiology fellows with invaluable opportunities to refine their technical skills, practice complex procedures in a risk-free environment, and strengthen their confidence before performing these critical interventions on patients. The high attendance and diverse skill stations demonstrate our fellows’ commitment to excellence and continuous learning in cardiovascular medicine.
In-Situ Simulations: Real Training for Real Emergencies!

Experience emergency training like never before! Our in-situ simulations bring realistic practice directly to your workspace. These sessions give your team the opportunity to practice real-life emergencies, strengthen communication, and identify system gaps before they affect patient care. By building confidence and teamwork, in-situ simulations are helping us advance both patient safety and our culture of continuous improvement.
In-situ simulations are offered system-wide—in both inpatient and outpatient settings. Recent partnerships include code blue simulations at Habersham, Lumpkin and Braselton medical/surgical units. On the outpatient side, our simulation team has collaborated with the Imaging Center to conduct code blue simulations across all five locations.
Interested in an in-situ simulation for your department? New item | Request for Simulation
