On Thursday, March 5, the Emergency Medicine residency program completed its fourth annual simulated mass casualty incident (MCI) exercise. This large‑scale simulation brought together emergency medicine residents, faculty, subject matter experts and numerous hospital and community partners to create a realistic disaster response training experience.
Standardized patients portrayed individuals injured in the simulated incident, helping to create a realistic clinical environment for learners. Simulation educators Corey Hill and Yesica White completed specialized moulage training to apply lifelike injuries, further enhancing scenario immersion. Months of detailed planning and preparation went into coordinating the exercise and ensuring all participants were ready.
This year’s scenario and event details were created by Abby Banks‑McClelland, a recent graduate of the Emergency Medicine residency program. Abby is currently completing a Disaster Medicine fellowship at UT San Antonio. She worked alongside Lead MCI GME Simulation Educator, Leah Everett, to design and implement the training. This year’s exercise focused on an anthrax exposure scenario, highlighting the recognition, triage and treatment of patients affected by a biological threat.
Key takeaways include:
- Enhanced disaster readiness: Residents practiced triage, rapid decision-making and patient management during a simulated mass casualty event.
- Interagency coordination: The exercise highlighted the importance of collaboration between hospital teams, EMS, law enforcement and emergency management partners.
- Operational understanding: Participants gained insight into incident command structure and the administrative coordination required during disasters.
- Realistic simulation training: Standardized patients, moulage and detailed planning created an immersive learning environment.
- Teamwork and leadership: Residents strengthened communication, prioritization and resource-management skills under pressure.
Several residents reflected on the value of the experience:
- “This year it was nice to be able to get into the administrative side of the MCI rather than the clinical portion of medicine.”
- “The MCI was very realistic. I learned more about what to prioritize and how to utilize resources.”
- “The whole entire event was useful!”
These reflections highlight how immersive simulation allows residents to move beyond theoretical disaster training and develop the practical leadership, coordination, and critical thinking skills required during real-world mass casualty incidents.
Mass casualty incident training is critically important in preparing emergency medicine physicians to respond effectively during disasters. Exercises like this allow residents to practice clinical decision‑making, communication, triage, and teamwork in a high‑pressure environment that closely mirrors real‑world events. By participating in these simulations, residents gain valuable experience that strengthens their readiness to lead and provide care during large‑scale emergencies.
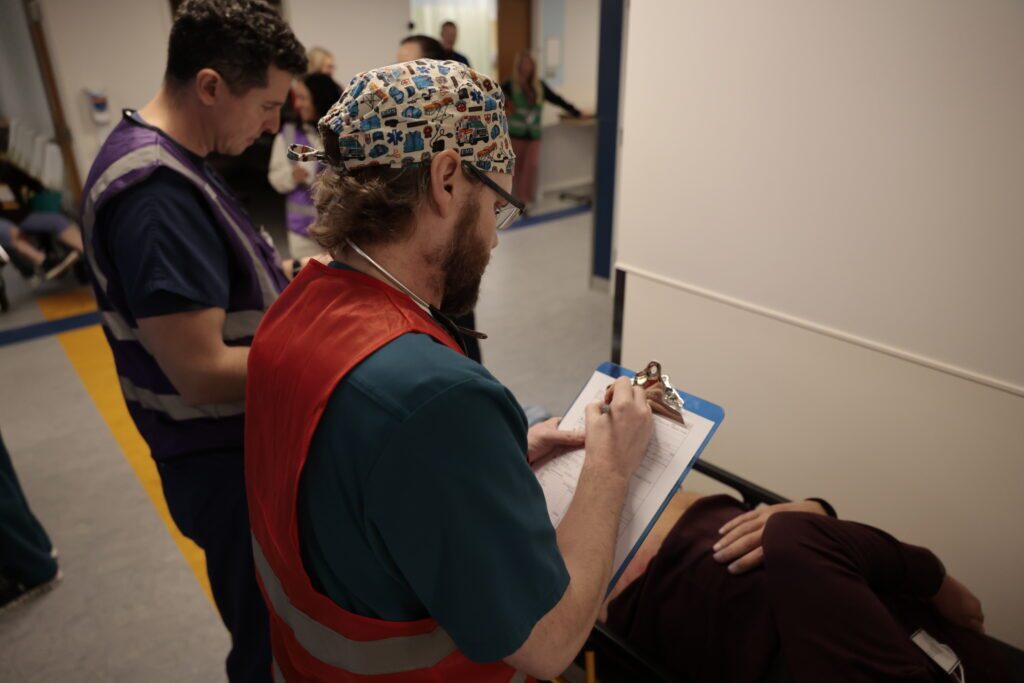





It takes a village…
The event required extensive collaboration across many departments and agencies, including emergency command, dispatch, transport services, law enforcement and fire services. Within the hospital, frontline nursing staff, sepsis coordinators, the simulated administrator on call and additional support teams played critical roles in ensuring the success of the exercise.
We also want to acknowledge the outstanding leadership of Dr. Josh Mugele, Emergency Medicine Residency program director; Dr. Sid Nagrani and Dr. Spencer Masiewicz, EMS medical director, whose support and guidance were instrumental to the success of this event.
In addition, we extend our appreciation to our community safety and emergency response partners, including Jay Parrish, City of Gainesville chief of police, and Zach Brackett, director of emergency management & homeland security for Hall County Government, whose collaboration and expertise strengthened the realism and operational depth of this year’s exercise.
We would also like to recognize key leadership within incident command, including Erick Giraldo, director of emergency medical transport for the health system; Greg LeMaster, manager of EMS operations; and Luke Anderson, emergency preparedness manager, for their coordination and oversight.
We would also like to acknowledge the simulation team for their contributions and leadership, especially Nicole Beringson, patient simulation manager and James Rinehart, director of GME Simulation & Clinical Skills, whose support and operational oversight were essential. The success of this exercise would not have been possible without the entire simulation education team and Simulation Educator Nicole Drury, whose months of planning, attention to detail and commitment to realism created an immersive and impactful learning environment for all involved.
Learn more about the Emergency Medicine residency and the Center for Simulation and Innovation.
